The dark history of the deadly SC opioid epidemic begins at a Myrtle Beach pain clinic

READ MORE
Pain Killer Beach
Twenty years ago in Myrtle Beach, authorities shuttered one of America’s first “pill mills.” No one knew the nation’s opioid crisis was just getting started.
Expand All

The dark history of the deadly SC opioid epidemic begins at a Myrtle Beach pain clinic

A pain clinic pill mill sparked an epidemic in SC. Where are the ‘Myrtle Beach eight’ now?

From patients to addiction, ‘a mess’ plagued victims in fallout of SC pill mill closure
From OxyContin to fentanyl, Myrtle Beach’s current drug epidemic is ‘larger than ever’
Myrtle Beach had no shortage of popular tourist attractions, so it was curious that throngs of out-of-town visitors were choosing to spend their time outside a doctor’s office.
Anyone walking past the pain clinic, tucked inside a strip mall along North Kings Highway, could see this was the place to be.
Major newspapers from far away chronicled the scene: a line of patients, 20 deep, snaked out the door and cars jammed the parking lot, morning and night. Next door, groggy patients waited at a hot dog restaurant, sometimes falling to the floor as they tried to hoist themselves onto stools at the counter.
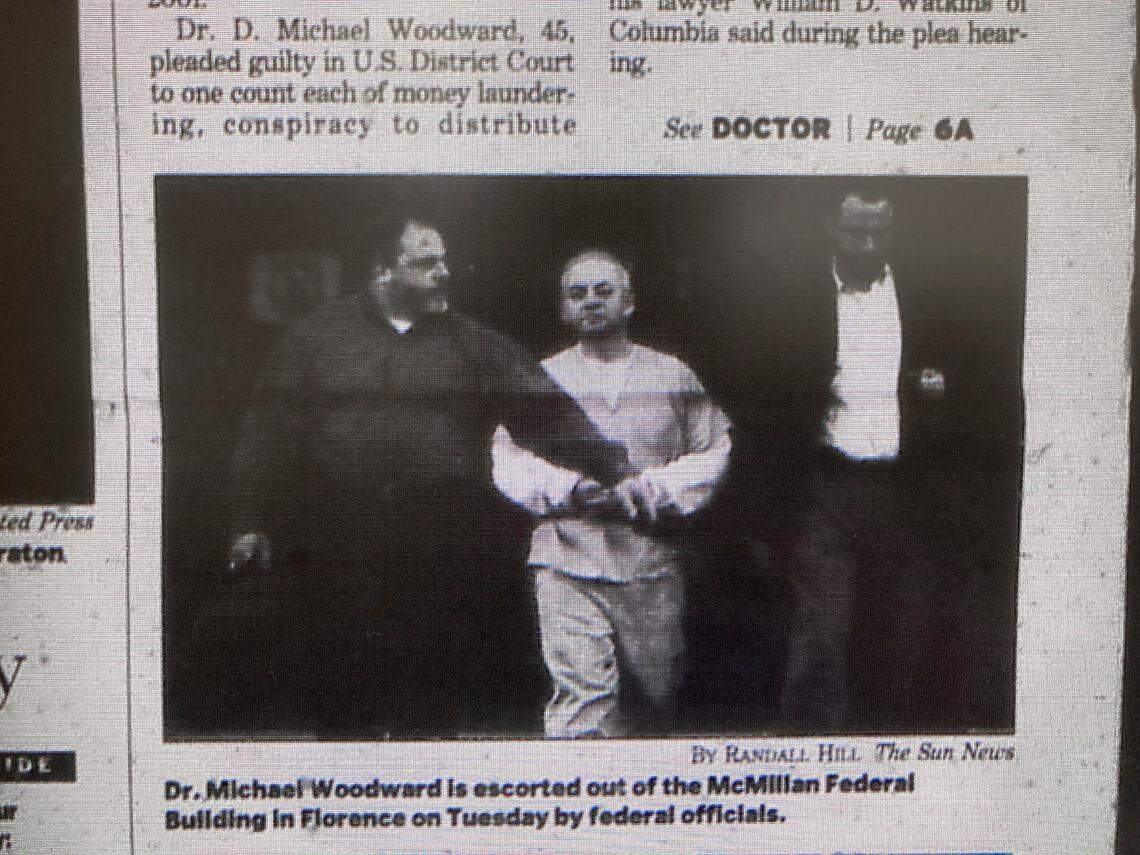
While everything happening on the outside looked suspicious, the real trouble was inside the clinic, run by Dr. David Michael Woodward.
In June 2001, authorities shut down Comprehensive Care and Pain Management Center and slapped Woodward and seven other physicians with federal charges for their unscrupulous peddling of OxyContin, a highly addictive painkiller.
Twenty years later, the end is in sight for Purdue Pharma, the bankrupt OxyContin maker often blamed for igniting the country’s opioid epidemic. To mark the milestone, The Sun News is looking back at Myrtle Beach’s unique role as home to Comprehensive Care, one of the country’s first and most notorious “pill mills.”
The clinic’s closure was not the end. An ensuing trial, centered on Woodward, the clinic’s mafia-connected physician who had a penchant for both assault rifles and powerful pain meds, captivated the nation’s attention.
More importantly, the trial served as a watershed moment that opened American eyes to a national opioid crisis just getting started in nondescript pain clinics like Comprehensive Care. Myrtle Beach was recast as a central figure in the nation’s pain-pill problem that has only grown in the 20 yeas since. Heroin and fentanyl soon took the place of OxyContin. Some 500,000 Americans have died since 1996 of opioid overdoses, making it the leading cause of accidental death in the country.
Looking back to 2001, the onset was sudden. Few predicted that a national crisis would soon unfold.
“One day we’re riding along and the road is (smooth), then all of a sudden we start hitting bumps in the road, and people are dying in their homes from these prescription drugs,” recalled Robert Edge, Horry County’s coroner for the past 30 years.
“It took a little while for everybody to catch on, but when we did, … some pressure was put on to start scrutinizing these pain clinics and try to slow them down.”
Lives were at stake — including at least five overdose deaths linked directly to Comprehensive Care.
“There was no doubt, just in this community, it was an epidemic,” said Dr. Brian Adler, a Surfside Beach internist who specializes in addiction treatment.
Opening up shop
Woodward was the valedictorian of his northwest Georgia high school — and a stickler for doing the right thing, his mother said.
“He was never a troublemaker,” she told The Sun News in a 2003 interview. “To my knowledge, he never even had a speeding ticket.”
After high school, Woodward, dark-haired and trim, earned both a master’s degree in business administration and a law degree. He then tried for seven or eight years before being accepted to medical school at Mercer University in Atlanta where he graduated in 1989, his mother said.
In 1993, he applied for a medical license in neighboring South Carolina. “I … plan to offer the best care possible to the people of the community,” he wrote in his application.
Woodward purchased a building within a year of arriving in Myrtle Beach and opened up the Carolina Neurodiagnostic and Sleep Disorders Center. But he soon realized the profit was in pain, later testifying that many new patients were threatening to leave if he didn’t prescribe narcotics.
Woodward went along with their requests, changing his practice’s name to Comprehensive Care and Pain Management Center.
But operating the clinic soon became impossible for Woodward to do by himself.

South Carolina suspended his medical license in 1996 after he was accused of improper relationships with female patients and overprescribing opioids, preventing Woodward from continuing to write his own prescriptions. So he hatched a plan.
He began recruiting and training other doctors to sign off on his prescriptions, eliminating the need for a valid license of his own, according to William “Bill” Day, a former assistant attorney for the U.S. Attorney’s Office in Florence who served as the lead prosecutor in the case against the doctors.
Among his recruits, there was Dr. Ricardo Alerre, a retired Air Force lieutenant colonel originally from the Philippines, looking to stay busy in between visits from his 14 grandchildren.
And Dr. Venkata Pulivarthi, who was born in a coastal village in India with a population of less than 3,500. He moved to the United States in the late 1980s, working short stints at hospitals in New York and North Carolina.
And Dr. Benjamin Moore, who was following in his grandfather’s footsteps as a physician, even graduating from his alma mater at University of North Carolina-Chapel Hill. Moore faced some unfortunate luck early in his career, working for three separate clinics in California and North Carolina that went bankrupt, leaving him with no insurance or savings to help pay off his sizable medical school loans.
Most of those recruited were facing difficult circumstances before arriving in Myrtle Beach, a judge later observed.
“They were down on their luck, if you please,” a 2007 appeals court opinion stated. “They were certainly not the most successful doctors around. (Woodward) picked them, put them down there, put them on their feet and gave them a way to make money.”
The doctors cycled in and out of the clinic, some of them leaving after only a few months. But the patients kept pouring in from across the state as word spread that Comprehensive Care was handing out prescriptions “like it was candy,” former patient Jennifer Altman recently told The Sun News.
Gerald Ghent, a patient and admitted drug abuser from Lancaster, was at one point driving carloads of others addicted to narcotics from the Upstate to the Myrtle Beach clinic in exchange for half of the painkillers they were prescribed, according to his testimony at trial.
In order to fulfill demand, the doctors perfected a practice called “fast-tracking,” Day explained. Multiple patients were gathered into a room with a single physician who granted each a prescription with minimal examination.
Dr. Deborah Sutherland, one of the clinic’s physicians who was later charged, said she was seeing as many as 80 patients in a day.
“I prescribed more [opiates] in two weeks than I did in my whole career,” she testified.
Opioid maker warned
Roddy Williams was growing suspicious.
Customers were routinely walking into his Surfside Beach pharmacy with prescriptions for as many as 240 OxyContin pills at a time. Comprehensive Care doctors were almost always the prescribers. (By comparison, narcotics prescriptions nowadays are limited to 15 pills at a time except in situations involving terminal illnesses, Adler noted.)
Williams, still the owner of Ocean Lakes Pharmacy, started telling certain customers he was out of stock. And he alerted the area’s Purdue Pharma sales rep about his concerns.
“I think (the sales rep) told me I had an obligation to fill a prescription,” he recently recalled. “I said, ‘No, I have an obligation to fill what I feel is a proper prescription.’”

The clinic’s physicians were prescribing other addictive opioids too, including Valium and Stadol. But OxyContin was overwhelmingly their prescription of choice.
Purdue Pharma’s first-quarter sales in 2001 for the sales territory including Myrtle Beach increased by more than $1 million, the most in the country, according to data obtained by The New York Times. As much as 40% of those sales originated at Comprehensive Care.
The surrounding community felt the clinic’s impact too.
Distribution of the painkiller tripled from 1999-2000 in the Myrtle Beach area, according to the Charlotte Observer.
And the clinic was clearly the primary culprit. The amount of OxyContin distributed by South Carolina pharmacists dropped from 217 grams per 100,000 people in 2000 to 91 grams in the months following the clinic’s closure, previous Sun News reporting showed.
In response to criticism at the time related to Comprehensive Care, Purdue Pharma officials told various media outlets that it had no data to suggest anything unusual occurring in Myrtle Beach. The inflated sales figures could be attributed to an older population more in need of pain medications, the company suggested.
Day, the prosecutor, told The Sun News his office had started to look into Purdue Pharma as part of its investigation at the clinic, but didn’t feel they had enough information to seriously pursue a criminal investigation back then.
Sutherland, one of the clinic’s doctors, recalled a Purdue sales rep assuring her the drug was not addictive because of its time-release feature — and pressured her to up the dosages, she later testified.
“If I had known then what I know now about OxyContin, I never would have prescribed it, and it’s my belief that I never would have gone to jail,” Sutherland told a federal grand jury, according to The New York Post.
The pharmaceutical company has since faced numerous charges and lawsuits, first pleading guilty in 2007 to misleading the public about OxyContin’s abuse potential, and it is currently in the final stages of a bankruptcy plan that could absolve the company and its owners of all future civil liability.
Extradition and suicide
Deputy U.S. Marshal John Radney, on a muggy July afternoon in 2002, pounded on the apartment door he’d been surveilling for about a week.
U.S. Drug Enforcement officials had closed Comprehensive Care a month earlier by suspending the remaining physicians’ medical licenses, and now law enforcement was rounding up the “Myrtle Beach eight,” as they would be referred to in media coverage.
Seven of them were easily found and arrested, including Woodward, who had moved to Florida with his wife and three kids to “escape the pressures of his profession,” he had told his mother.
But Sutherland was still at large, and Radney had tracked her to her listed address in Columbia. He was greeted by her husband, William Drake, who told him a story that was difficult to believe.
Drake insisted his wife had left him and was seeking employment as a doctor on an American Indian reservation or in Rockview, Maryland, according to a federal affidavit from the marshal.
Further attempts to locate her elsewhere in the United States were fruitless, the affidavit states.
A month later, investigators sought the assistance of the U.S. Department of State and found that she had received a permit to work at a health clinic in a small village in New Zealand called Maori, and she was taken into custody there.
Sutherland fought extradition, according to previous Sun News reporting, and Day recalled that getting her back was difficult because she was one of the only doctors in Maori, and they didn’t want to let her go.
Authorities were able to successfully extradite Sutherland in December 2002, shortly before the trial was set to begin, and she decided to plead guilty, becoming the fourth doctor from the clinic to do so — joining Drs. Benjamin Moore, Thomas Devlin and Venkata Pulivarthi.
Those four were expected to testify against their former colleagues as part of their plea agreements, Day explained, but Moore never made it to trial.
Facing up to 45 years in prison, the 44-year-old committed suicide while living with his mother in North Carolina.
“Theoretically if the penalty were a mandatory death sentence, then I would rather go to trial,” Moore wrote in a letter explaining his decision to plead guilty. “I’m not as afraid of death as I am loss of freedom.”
Moore gained notoriety after his death, becoming a symbol in the “War on Doctors” movement. Its advocates argued that government officials were wrongly placing the blame for the opioid epidemic on physicians like Moore. They warned that unnecessary prosecutions of doctors who were acting in the best interest of their patients would discourage others from treating chronic pain.
The movement spawned online forums, protests and books during its early 2000s heyday.
“(Dr. Moore) became entangled in the vast web that is our legal system and was helpless against the power, resources, and cunning of predatory government agents,” wrote Siobhan Reynolds, a leading advocate for the movement, in her blog. “Perhaps, Dr. Moore, we will some day present an annual award memorializing you, for (being) the bravest doctor in Pain care in America.”
The man behind the SC clinic
With the trial approaching, the doctors who already pled guilty were painting Woodward as an intimidating figure.
A cache of 21 guns, including at least five AK-47 military-style weapons, and 17,000 rounds of ammunition investigators confiscated from Woodward’s office, enhanced the perception that he might be dangerous.
Authorities never received an explanation as to why he kept so many guns in his doctor’s office, Day recalled.
Woodward had also warned his employees that he was connected to the mafia, a DEA investigator later testified.
That assertion turned out to be true, as he was leasing space within the clinic’s building to an MRI scanning company run by Joseph LoCascio, whose brother served as second-in-command for the infamous New York mobster John Gotti, court records show.
Woodward provided evidence against the business in an effort to reduce his prison sentence.
LoCascio and others associated with the business would plead guilty to health care fraud after paying Woodward more than $300,000 in kickbacks to refer patients for unneeded MRI scans.
Prosecutors, however, encountered a pleasant, affable man, who didn’t seem to fit the shadowy characterization.
“The side I saw of (Woodward) was easy to get along with, very cooperative,” Day said at the time. “He wasn’t the least bit hostile. A lot of people had been afraid of him and his temper, but I didn’t see that.”
Less than three weeks before the trial was set to begin in January 2003, Woodward thought better of facing a jury, becoming the fifth doctor to plead guilty and forfeiting the $640,000 he’d made from the sale of the clinic.
The three remaining physicians — Drs. Ricardo Alerre, Deborah Bordeaux and Michael Jackson — now had to grapple with their former boss serving as the prosecution’s key witness.
A guilty verdict
Taking the stand on the fifth day of trial, Woodward laid out in vivid detail his alleged scheme, which netted the practice about $6 million from 1997 to 2001.
Each of his fellow doctors had an important role to play, and the three staring daggers at him now had all implicitly agreed to be “part of the team,” he recalled.
“I got your back,” Jackson had told Woodward after the clinic owner showed him how the cursory exams were conducted and asked if he was on board.
A similar exchange with Bordeaux ended with her asking for Woodward’s father’s pickup truck in exchange for her cooperation, he told the jury.

Facing cross-examination from the defense, Woodward estimated 15 to 20% of patients had real issues that benefited from the narcotics, but that would’ve been purely coincidental because every patient was treated the same.
Despite noble intentions when he first entered the medical profession, Woodward was now ready to admit that his clinic had indeed become a “pill mill.”
The jury heard testimony from 54 witnesses during the three-week trial, but Woodward’s six hours on the stand were incriminating enough on their own to find the defendants guilty, an appeals judge later ruled.
The doctors waited seven hours before the jury was ready to announce its verdict: all three were guilty of illegally distributing narcotics, a decision “which the defendants received in stunned silence,” The Sun News wrote in February 2003.
“Dr. Woodward was coerced into plea bargaining against the other physicians, including myself,” Jackson told Inter Press Service in 2006. “He perjured himself by implying that there was a conspiracy to distribute opioids illegally.”
Day said he was happy with the result at the time. But the lid of Pandora’s box had swung open, he realized, and there was no forcing it shut now. His successful prosecution, he knew, would hardly make a dent.
The proof was soon everywhere.
Other local doctors were understandably wary of filling the pain clinic’s void. Comprehensive Care’s abandoned patients filled emergency rooms, suffering through painful withdrawals or buying cheaper alternative narcotics off the streets, recalled Adler.
“There were lots of people whose lives were ruined as a result of the opiate climate back in that time,” he said.
States, counties and cities all over the country have declared states of emergency during recent years in response to the ever-increasing overdose death counts and costly treatment needs. The epidemic has shown no signs of slowing down.
“Unfortunately I wish I could say it (got) better, but it’s probably as bad now, if not worse.”
Read next: A pain clinic pill mill sparked an epidemic in SC. Where are the ‘Myrtle Beach eight’ now?
This story was originally published October 7, 2021 at 5:00 AM with the headline "The dark history of the deadly SC opioid epidemic begins at a Myrtle Beach pain clinic."
