As NC moves to reopen, COVID ICUs at Rex Hospital expect to remain busy for awhile
Rex Hospital admitted its first COVID-19 patient on March 19 and a week later opened a new intensive care unit just for people made ill by the novel coronavirus.
No one knew then how the coronavirus outbreak would play out in North Carolina. Would hospitals be overwhelmed with patients struggling to breathe, the way they were in China, Italy and eventually New York? Would they run out of equipment, staff or beds to treat people with a contagious disease doctors had never seen before?
The Special Respiratory Isolation Unit, or SRIU, was one step UNC Rex Healthcare took to get ready. It revived a former cardio-thoracic ICU that was being used for storage and installed a new air handling system so the rooms have negative pressure, a slight vacuum that means nothing from the unit would spread to the rest of the hospital.
The eight patient rooms in the ward were equipped with ventilators and other specialized equipment. Everything was configured so that the unit could handle up to 16 infectious COVID-19 patients, two per room.
“That’s not the preference,” says Anastasia Jennings, a critical care nurse who manages the SRIU, about doubling up. “That would only be if we were in a disaster state and Raleigh was overrun with patients.”
So far, that has not happened. The surge of patients that hospitals across the state prepared for hasn’t arrived, something hospital and public health officials credit to efforts to keep people home and physically apart. Instead, hospitals have seen a steady but manageable number of COVID-19 patients that has fluctuated between 300 and 550 statewide since early April, according to the state Department of Health and Human Services.
Rex had admitted a total of 48 COVID-19 patients as of Thursday. In addition to the SRIU, it converted a nearby neuro surgical ICU into a second 10-bed COVID ward in April, and the two units have been able to handle nearly all the coronavirus patients at Rex, each with their own room.
Three COVID-19 patients have died at Rex, said UNC Health spokesman Alan Wolf, part of the statewide death toll that topped 500 on Thursday. Twenty were still in the hospital, but the majority of the hospital’s coronavirus patients — 25 so far — have gotten well enough to leave, including all that have come through the SRIU.
“Normally with gravely ill people you do expect to see some mortality; unfortunately not everybody always gets better,” Jennings said. “So it’s been really great to see that happen here, where these patients were very, very sick, and then got better and were able to go home and have celebrations.”
The intercoms at hospitals occasionally broadcast alerts that summon staff for an emergency — Code Blue for a patient whose heart or breathing have stopped, for example. Rex now has a Code Rocky, which calls staff who are able to line the main hallway near the exit when a coronavirus patient is being discharged.
The first Code Rocky went out April 28, and hospital staff expect they will continue for months.

Not a normal intensive care unit
Intensive care units are normally reserved for the most critically ill patients who need specialized care and more attention from nurses and others. But while all of the people in the SRIU are sick enough to require hospitalization, their conditions vary. As patients get better, they remain in the intensive care unit to keep them isolated from other patients and staff right up until they leave the hospital.
In addition to doctors, therapists and other health care workers who pass through, 22 nurses and nursing assistants are assigned to the SRIU. An average of five are on duty at any given time, working 12-hour shifts three days a week. Jennings says she’s usually there about 50 hours a week but is on call 24/7 and answers calls and emails at all hours.
Everyone wears at least a surgical mask, but those who work with patients alternate between two other types.
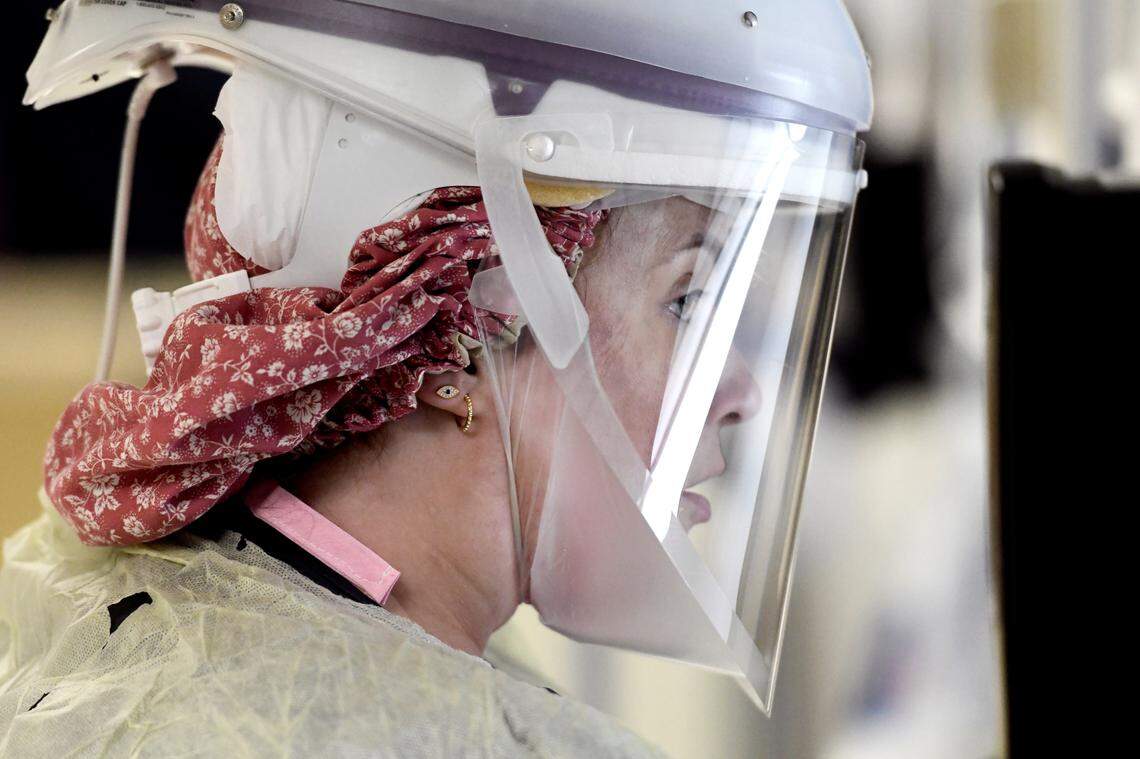
The N95 is a tight-fitting respirator mask designed to prevent at least 95% of airborne particles from being inhaled, but it can bruise the bridge of your nose if you wear it long. The other is the MAXAIR, which looks like a bicycle helmet with a sealed face shield and a small motor that draws in and filters air and blows it down across the face. It’s supposed to keep out 99% of particles but is heavy and hard on the back and shoulders after a while.
Alana Goodale, a registered nurse, says working in a mask all day doesn’t bother her. Goodale volunteered to work in the SRIU because she likes the challenge of helping patients critically ill with a disease people don’t fully understand. She says if she had been around when HIV and AIDS were emerging she would have wanted to care for those patients, too.
Goodale has worked with tuberculosis and other infectious diseases and doesn’t worry about contracting COVID-19.
“I was always taught to respect it and not fear it,” she said. “So as long as you’re prepared, that’s all you can do.”
Each patient room has sliding glass doors, and only staff who need to go in do, sheathed in gowns, gloves and masks to limit their exposure. Patient needs range from the serious to the mundane; at one point Wednesday afternoon, an echocardiogram machine was wheeled into one room to check a patient’s heart while a nurse brought cups of shampoo and conditioner into another so a patient’s hair could be washed.
Jennings said the unit doesn’t look or feel the way hospitals in New York and elsewhere have appeared on TV or the internet.
“We have had times like any critical care unit where it’s busy and there’s lots of things going on and some things aren’t good and it may look chaotic,” she said. “But most of the time we have enough staff and resources to maintain a very quiet or therapeutic environment for the patients as well as the staff.”
Learning about COVID-19 as they go
COVID-19 emerged only a few months ago, and health care workers all over the world are still learning about the disease and how to treat it. That’s true at Rex as well.
For example, Rex has found that about a quarter of COVID-19 patients need continuous renal replacement therapy or CRRT, a filtering of the blood similar to dialysis. When staff noticed that the filters on the machines were getting clogged, Jennings said, they responded by giving patients blood thinners and adjusting the rate of filtration.
“When you’re taking care of patients that have the flu, for instance, the flu’s been around for decades,” Jennings said. “But COVID-19, it’s new and we learn about different symptoms and how to treat patients the best as time goes on.”
As North Carolina prepares to gradually lift restrictions that have closed businesses and restricted people’s activities, the two COVID ICU units at Rex are full. On Wednesday, a floor of patient rooms that Rex had set aside for overflow coronavirus patients was opened for the first time.
While the feared surge of coronavirus patients has not materialized, Rex and other hospitals in the region say they remain prepared for one. In any event, they expect to be treating COVID-19 patients for the foreseeable future and say the relatively slow growth of the virus in North Carolina has helped them get ready for whatever comes next.
“It’s kind of got us at a good point where we can prepare and better understand the disease,” said Goodale, the registered nurse. “Whereas other places like New York and New Orleans, they got hit so hard, it’s hard to keep up with everything at that point. So this has been a good thing for us. And it’s been nice to see these patients leaving.”
This story was originally published May 8, 2020 at 6:00 AM with the headline "As NC moves to reopen, COVID ICUs at Rex Hospital expect to remain busy for awhile."
