‘Continued vigilance’: Face masks contribute to decline in COVID-19 cases in Horry County
Health experts have been advising folks to wear face masks since March to slow the spread of COVID-19, but without a state mandate in South Carolina, local municipalities began taking action in July.
After coronavirus cases began to spike in Horry County in June, resulting in S.C. Department of Health and Environmental Control labeling the area a hotspot for the virus and the area receiving national press coverage, most Myrtle Beach-area municipalities began enforcing their own mandates requiring masks be worn just before the July Fourth holiday weekend.
And it appears the act of wearing a mask or covering has aided in cases decreasing significantly.
“There’s a direct correlation between mask wearing and the decline (in cases) and I don’t doubt that any public health official would deny that,” said Gayle Resetar, chief operating officer at Tidelands Health. “The only reason we’re really seeing a decline is because we’re controlling the spread. The disease is not gone by any stretch of the imagination.”
On Wednesday, Horry County saw its lowest daily case total recorded since early June, at 24. A month prior on July 12, DHEC announced there were 208 new cases in the Myrtle Beach area. On July 4, cases peaked reaching a daily high of 358.
Prior to the area hosting its first testing event on May 30, Horry County had reported 426 coronavirus cases since the first case was reported on March 15. Since May 31, Horry County has seen 8,376 COVID-19 cases, as of Saturday.
With cases mainly reported in the triple-digits in the month of June and July, confirmed positive cases began to see a sharp decline toward the end of July, despite the occasional triple-digit caseload, according to DHEC. Since the start of August, cases have remained on a downward trend.
With the exception of Aug. 7, when 115 new coronavirus cases were reported in Myrtle Beach, the month has recorded only double-digit numbers. As of Saturday, Horry County reported a total of 8,802 confirmed cases of coronavirus and 162 deaths.
Do masks work? Here’s what the data shows
Since mask mandates were put in place across Horry County, the area has seen a dramatic slow down of COVID-19 growth, after seeing explosive rates before mask rules were in place, The Sun News found, comparing COVID-19 case data before and after the rules took effect just before July 4.
The Myrtle Beach area reported 1,525 new coronavirus cases between June 29-July 5.
Between July 6-July 12, there were 1,311 confirmed new cases in Horry County, with that number dropping by 385 the following week to 926 cases. There were 733 new cases reported between July 20-July 26, with the number decreasing again to 641 the week of July 27-Aug. 2.
Between Aug. 3-9, there were 471 new cases of coronavirus reported in Horry County, according to DHEC.
Since Monday, there have been 144 new cases, with the area seeing cases drop to 24, the lowest daily case total since the start of June. However, while there are currently 8,802 reported cases in Horry County, DHEC estimates there’s more than 62,000 possible cases in Horry County that have gone unreported or diagnosed.
“I definitely think the decline we’re seeing in Myrtle Beach is attributable to the mask order,” Myrtle Beach Mayor Brenda Bethune said. “The majority of people realize that masks are keeping them safe and those around them.”
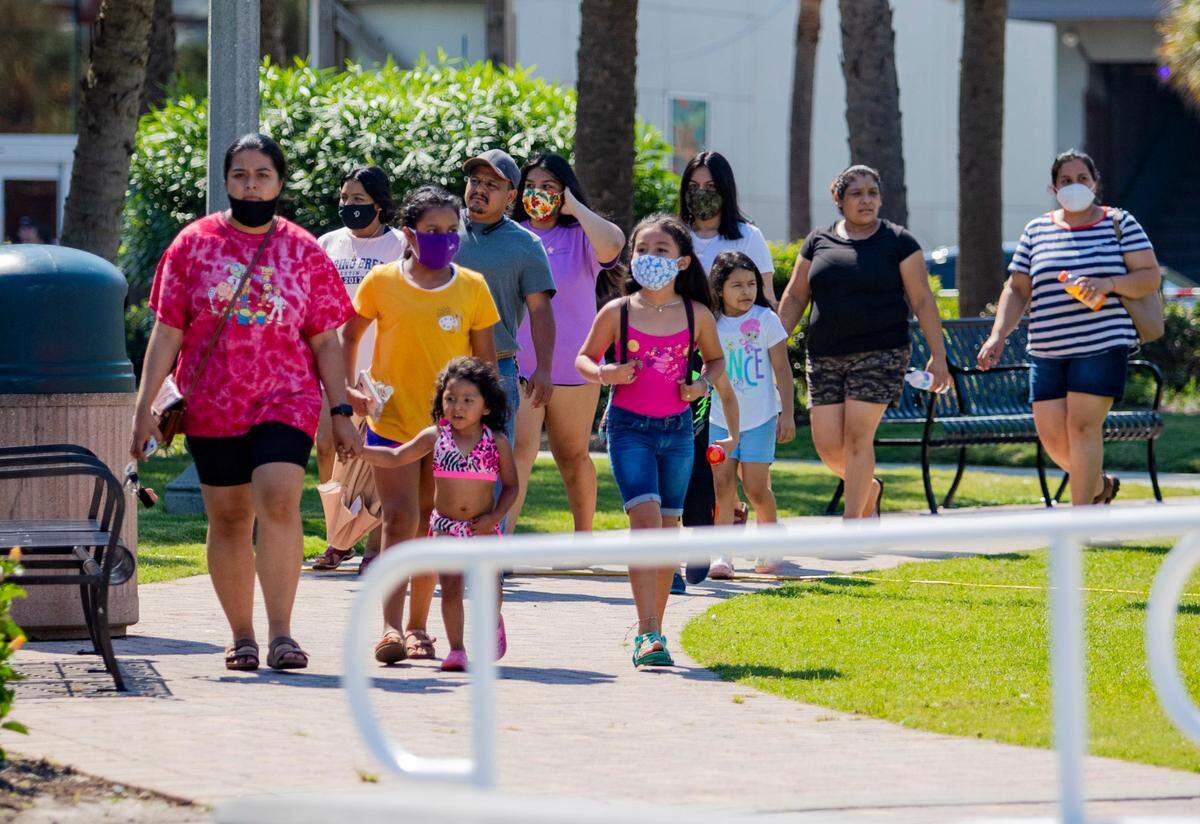
As coronavirus cases continued to boom in Horry County and the tourist destination started making national headlines amid the outbreak for its lack of regulations as thousands inundated Myrtle Beach for vacation, local leaders took action, approving mandates that require face masks or coverings in public places.
With the exception of Surfside Beach, which only recommends masks be worn, each municipal ordinance carries a different set of rules and fines. But places like Myrtle Beach, North Myrtle Beach, Conway, Horry County and Atlantic Beach similarly mandate masks be worn in places like groceries, pharmacies, restaurants, and anywhere social distancing can’t be adhered to.
The ordinances don’t apply to public parks or beaches.
Weeks later, S.C. Gov. Henry McMaster, who has strongly opposed enacting a statewide mask order, changed his tune requiring masks be worn inside state buildings, at restaurants and at other types of businesses where events are held or people gather en masse. He also advised local governments to enforce their own mask laws.
“These limited restrictions are temporary, they are measured, and they are targeted towards what we know works,” McMaster said in a statement on July 29. “These measures give South Carolina the best chance to slow the spread of the virus without shutting down the state’s economy — which we cannot and will not do — as many continue to call for.”
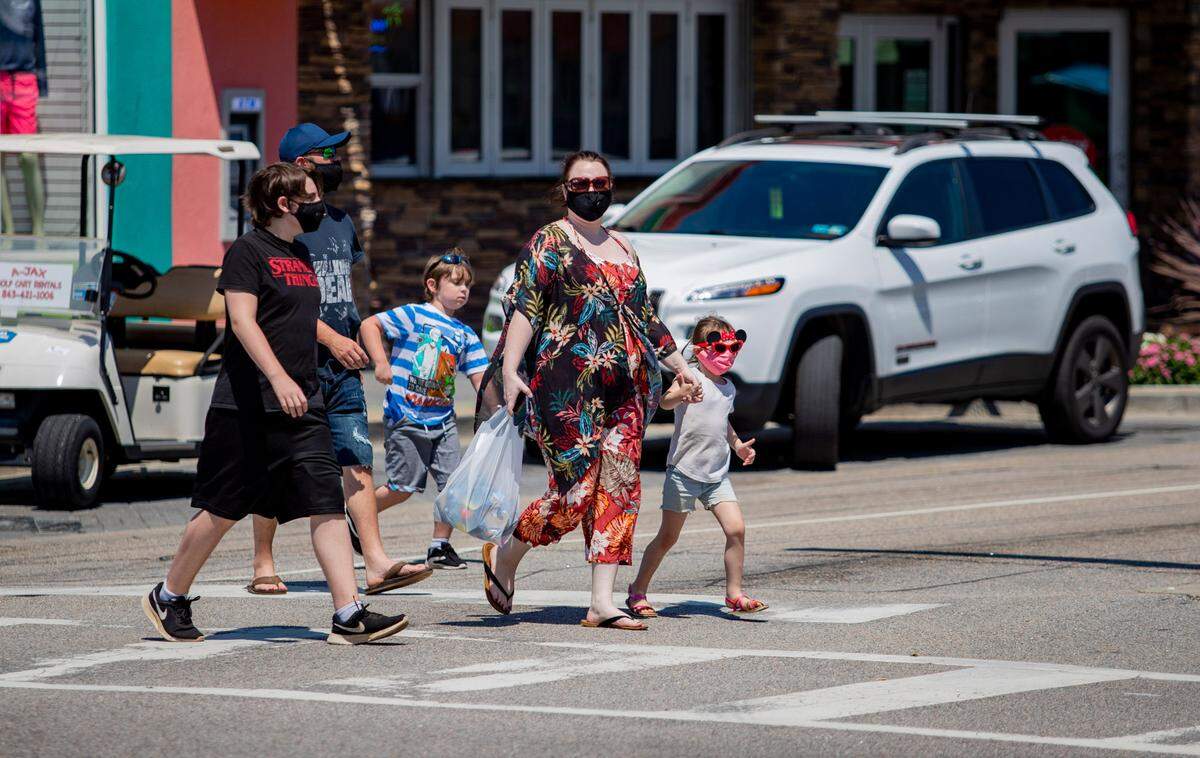
According to state and local health officials, mask orders across South Carolina have been effective in slowing the spread of the sometimes fatal virus.
According to DHEC, nearly 40 percent of state residents, or approximately two million, reside in jurisdictions that have local mask requirements in place, as of this week. When comparing the jurisdictions that have mask requirements in place to those that don’t, those with orders have seen a 46.3 percent decrease in the total number of cases, DHEC reports.
“This new data shows us what we already knew, wearing face masks works,” S.C. Epidemiologist Dr. Linda Bell said in a news release on Wednesday. “We’re strongly supportive of these local leaders’ initiatives that are centered on protecting the health and well-being of their communities.”
Cases low but deaths are high. What’s up with that?
While COVID-19 cases are seeing a downward trend in the Myrtle Beach area, deaths stemming from the virus are still seeing higher than normal numbers, but they are decreasing — slowly. Though, that is considered a normal trend.
Despite the rise in deaths, Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, has warned that “deaths always lag considerably” behind cases. He explained that as cases rise, deaths will remain minimal, but the opposite will occur when cases begin to see a decline.
Since July 5, weekly deaths in Horry County have been recorded in the double digits, with weeks prior seeing single-digit accounts, according to DHEC. The area’s highest daily fatality number reached a high of eight on July 28 and Aug. 4.
Between July 27-Aug. 2, Horry County recorded its highest number of coronavirus deaths in a single week at 25. There were 20 deaths reported the following week.
Between July 20-July 26, there were 19 new coronaviurs deaths, nearly doubling the amount of deaths in the previous week, with at least one death recorded each day of the week, according to DHEC.
The area saw 17 fatalities between July 6-July 12, with the previous week reporting 10 deaths, according to DHEC. Only two deaths were reported between June 22-June 28.
As of Saturday afternoon, there have been have 14 new deaths reported since Monday, according to DHEC.
Currently, there are 161 confirmed coronavirus-related deaths in Horry County. The area’s first death was reported on March 24.
‘We’re nowhere near out of the woods’
While cases continue to see a decline, it’s not an excuse to stop taking precaution, health experts say.
Resetar warned that residents should continue to remain vigilant in taking preventive measures, such as masking wearing, maintaining good hygiene, social distancing and avoiding large crowds. This virus is still very deadly, she said.
“We’re nowhere near out of the woods,” Resetar said, explaining that positive COVID-19 patients continue to be hospitalized everyday for treatment. “If people begin to let their guards down and reduce mask wearing just because numbers are down, there’s virtually no doubt the numbers will go right back up.”
There are currently no vaccines or antiviral drugs approved to treat COVID-19. Those who test positive for the coronavirus are advised to quarantine for 14 days or go to the hospital if symptoms worsen.
Currently, viral tests are used to diagnose COVID-19, with tests identifying the virus in respiratory samples, such as from swabs from inside the nose. Antibody testing is also available, with clinicians taking a sample of a person’s blood to look for antibodies to the virus that causes COVID-19.
However, experts don’t know yet if those who recover from COVID-19 can get infected again, according to the CDC. While researchers are racing to produce a vaccine, there’s no telling when one would become available to the general public for use, despite chatter among national leaders assuring one will be ready in 2021.
But with restrictions mainly lifted in states nationwide, health experts still urge the best way to prevent contracting the virus is to avoid exposure.
“It’s not over by any stretch, and we continue to see a lot of hospitalizations, there’s still mortality, and there’s still people who find themselves critically ill at all ages,” Resetar said. “There should be continued vigilance as we go into the fall, for sure.”
Here are some of the benefits to wearing a face mask
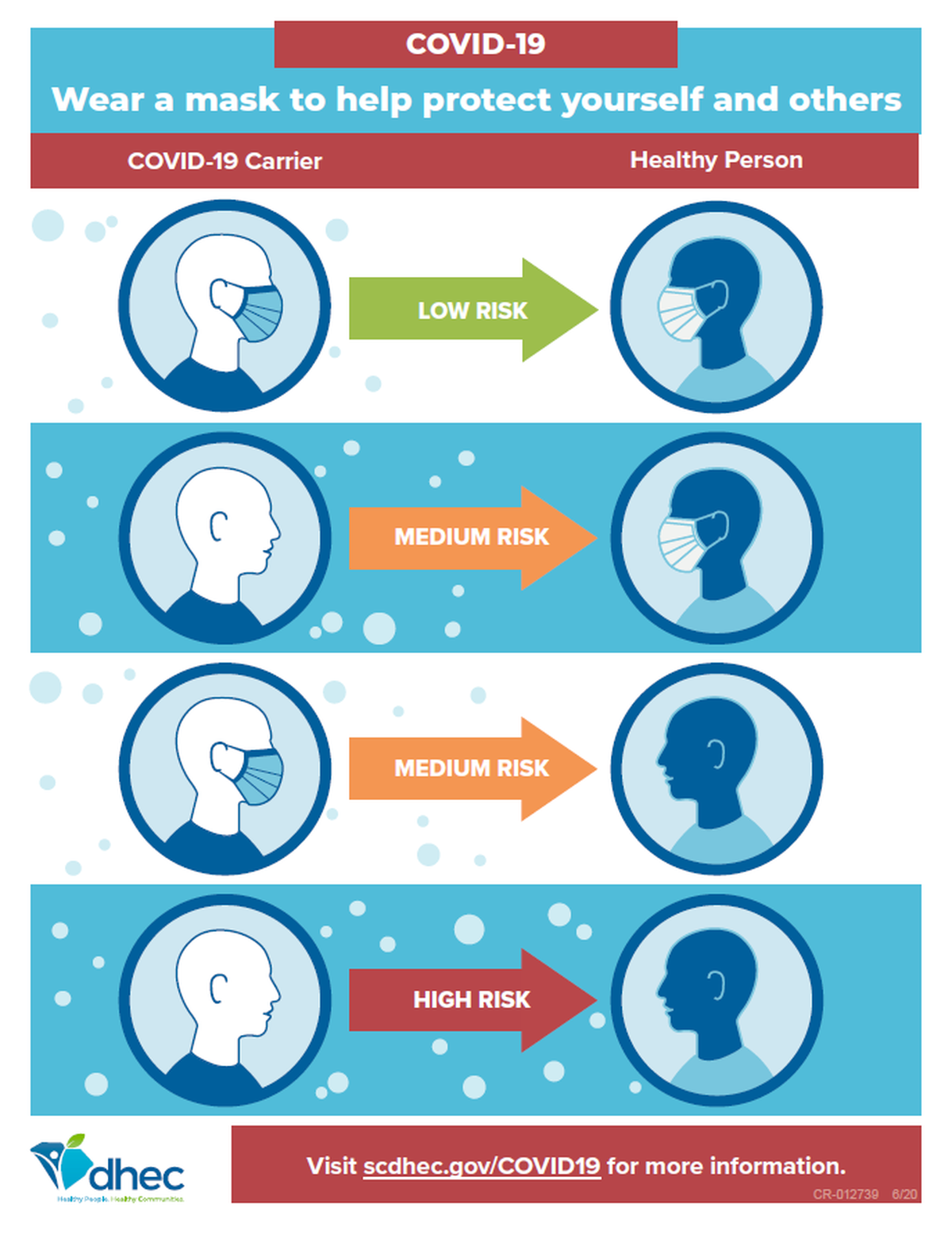
With no vaccine to help prevent the spread of COVID-19, the Center of Disease Control and Prevention recommends wearing face masks to avoid being exposed to the virus or spreading it to others if you’re infected but don’t have symptoms.
According to the CDC, a cloth face covering can provide an extra layer to help prevent the respiratory droplets from traveling in the air and onto other people.
Face coverings can include, but are not limited to, bandannas, medical masks, cloth masks, scarves, and gaiters, provided it securely covers the person’s nose and mouth. Homemade face coverings, similar to surgical masks, won’t necessarily prevent you from getting sick, but it can provide a barrier that may stop the spread of the virus to other individuals.
Other prevention methods include keeping a 6-foot distance between individuals, maintaining good hygiene, avoiding touching the eyes, nose and mouth, sanitizing and washing hands often with soap and water for at least 20 seconds, especially after frequenting a public place or sneezing, coughing or blowing your nose.
The coronavirus can spread through respiratory droplets released into the air when an infected person coughs, sneezes or talks, resulting in those droplets landing in the mouths or noses of people who are nearby, the CDC reports. The droplets can stay aloft within about 6 feet of the person, which is why social distancing is considered an effective model in averting the virus’ spread.
While face masks are recommended, the CDC makes exceptions for children under the age of 2 of anyone who has trouble breathing, is unconscious, incapacitated or otherwise unable to remove the mask without assistance.
“There’s a lot of evidence now out there on masking,” Resetar said. “You’re protecting the people around you as much as you’re protecting yourself.”
